A clean care environment is not just about appearance. It is a daily signal that infection control, patient safety, and proper standards are being taken seriously.
Key Takeaways:
- Healthcare-associated infections (HAIs) affect approximately 165,000 Australians each year, and inadequate environmental cleaning is a direct contributing factor.
- Cleaning frequency is not a fixed schedule. It is driven by risk category, surface type, patient vulnerability, and local infection pressure.
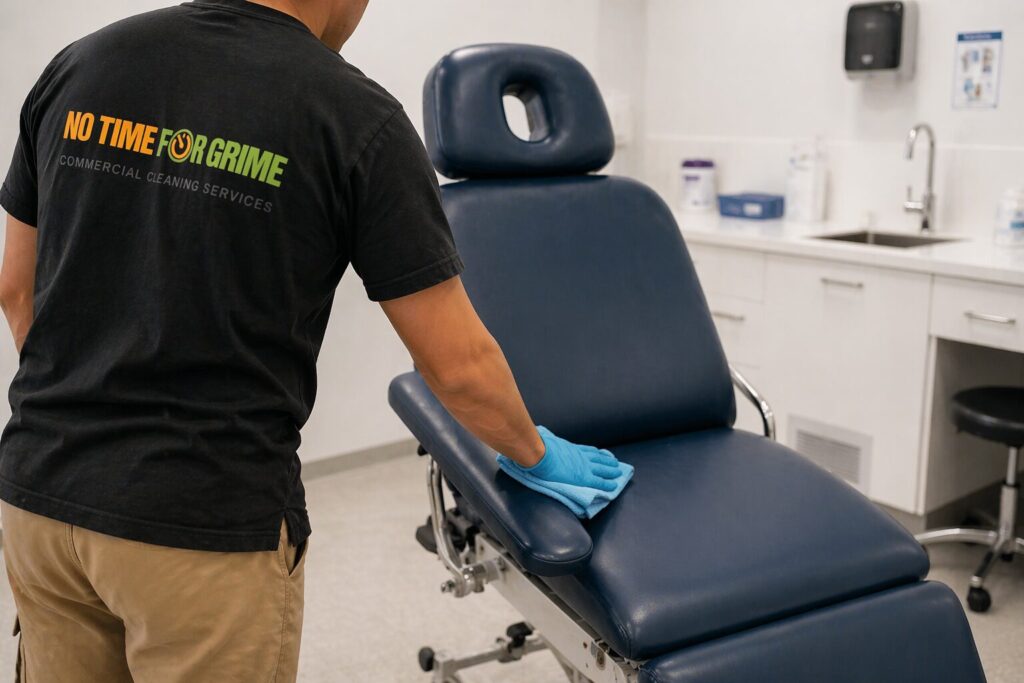
- High-touch clinical contact surfaces (bed rails, door handles, light switches, treatment chairs) must be cleaned at least daily with a detergent solution, and immediately after any contamination.
- Detergents remove soil and organic matter; disinfectants kill pathogens. Using a disinfectant on a dirty surface without cleaning first reduces its effectiveness significantly.
- Waiting room hygiene is often overlooked in smaller medical centres. Shared seating, reception surfaces, and reading material represent genuine transmission risks
I’ve been in a lot of medical centres over the years, not as a patient, but to audit cleaning standards and work through what’s actually happening on the floor versus what the cleaning schedule says should be happening. The gap between the two is often surprising, and in a healthcare setting, that gap has real consequences.
The question I get asked most often by practice managers and facility coordinators is a simple one: how often does everything actually need to be cleaned? It sounds straightforward. It isn’t. The answer depends on what surface you’re talking about, what’s happening in that space, and who’s using it. Getting this right is not just a compliance issue. It’s a direct infection control measure.
Why Healthcare-Associated Infections Are a Problem Worth Taking Seriously
Before we get into the practical side, it’s worth understanding what’s at stake. According to the Australian Commission on Safety and Quality in Health Care, healthcare-associated infections affect approximately 165,000 Australians every year. These are infections that patients and staff acquire in care settings, not the conditions they came in for. They drive up treatment costs, extend hospital stays, and in vulnerable patients, they carry a serious risk.
Environmental surfaces are not the sole driver of HAIs, but they are a consistent contributor. Pathogens can survive on hard surfaces for hours, and some for considerably longer. The problem is not always dramatic. It is often incremental: a treatment chair arm that gets wiped at the end of the day but not between patients; a waiting room that looks tidy but has touch points that haven’t been disinfected since the morning clean; a floor that gets mopped but where the mop head has not been changed between areas.
This is where a clear, risk-based understanding of cleaning frequency matters more than any generic schedule.

The Difference Between Frequently Touched and Minimally Touched Surfaces
Not every surface in a medical centre requires the same level of attention, and treating them all the same is both wasteful and ineffective. The Australian Guidelines for the Prevention and Control of Infection in Healthcare draw a clear line between two categories.
Frequently touched surfaces, including door handles, light switches, bed rails, treatment chair arms, reception counters, telephone handsets, EFTPOS terminals, and tap handles, need to be cleaned with a detergent solution at least daily and immediately after any visible contamination. In a busy GP clinic or specialist practice where patients cycle through quickly, “at least daily” often means multiple times across a shift.
Minimally touched surfaces, including walls, ceilings, floors, windowsills, and blinds, only need to be cleaned when visibly soiled or immediately after a spill. This is a point that surprises a lot of people. The floor in an exam room does not need disinfecting twice a day. It needs to be free of dirt, organic matter, and spills, and cleaned with detergent and water as required. Overuse of disinfectants on low-risk surfaces does not improve outcomes; it adds cost and increases the likelihood of chemical residue build-up.
The practical takeaway for any medical centre cleaning program: allocate your attention to high-touch clinical contact surfaces, and make sure your team knows the difference between them and the rest of the environment.
How Risk Category Should Drive Your Cleaning Schedule
In larger healthcare facilities, surfaces and functional areas are grouped into risk categories: extreme, high, medium, and low. Cleaning frequency is tied directly to that classification. A GP clinic or specialist rooms setting might not use that exact framework, but the underlying logic applies to every care environment.
High-risk areas include any space where invasive procedures take place, where immunocompromised patients are treated, or where there is regular exposure to blood, body fluids, or open wounds. These areas warrant more frequent cleaning, more careful product selection, and immediate response to any visible contamination.
Lower-risk areas like waiting rooms, staff offices, and corridors still need routine attention, but the frequency and the products used are different. A waiting room floor does not carry the same infection risk as a treatment room surface. What waiting rooms carry is a concentrated volume of potentially unwell people touching the same surfaces repeatedly: armrests, magazine racks, door handles, and reception counters. These are high-touch surfaces even in an ostensibly low-risk zone, and they should be cleaned accordingly.
One factor that elevates risk across the board is local infection pressure. If your area is seeing elevated cases of a respiratory illness, multi-resistant organism activity, or a gastroenteritis cluster, that context should push your cleaning frequency up, particularly for shared and high-touch surfaces.
Cleaning First, Then Disinfection: Why the Order Matters
One of the most common mistakes I see in clinical cleaning practice is reaching for a disinfectant as the first step. The logic seems sound: disinfectants kill pathogens, so they should be the primary tool. In reality, disinfectants do not clean. They cannot penetrate organic matter, and soil or bodily fluids on a surface will inactivate them before they can do their job.
The correct sequence is always: clean first with detergent and water to remove soil, then apply a disinfectant if the clinical situation requires it. This is what’s referred to as the two-step process. The alternative is a combined two-in-one detergent/disinfectant product, which handles both functions in a single application. These products are registered with the Therapeutic Goods Administration (TGA) and are suitable for general clinical contact surface cleaning where both cleaning and disinfection are needed simultaneously.
Not every surface requires disinfection as a routine measure. Queensland Health’s infection prevention guidelines make the point directly: disinfection of the healthcare environment is not always required. The clinical indication matters. Routine cleaning with neutral detergent and water is the appropriate default for most surfaces. Disinfection is indicated when a patient is known to carry a multi-resistant organism, when there has been a blood or body fluid spill, after the room has housed a patient with a transmissible infection, or when local epidemiology warrants it.
For any product that does make a disinfectant claim, it must be listed on the Australian Register of Therapeutic Goods (ARTG) before it can be used in a clinical environment. Always follow the manufacturer’s instructions on contact time. A disinfectant that is wiped off before the required dwell time has not done its job.
Managing Spills and Body Fluid Contamination Correctly
Body fluid spills represent the highest immediate risk in any care environment, and the response process is not complicated, but it needs to be carried out in the right order. The person managing the spill should have appropriate PPE on before they begin, at a minimum, disposable gloves and an apron.
For a significant spill, the surface needs to be contained first with a paper towel or an absorbent material, which is then disposed of as clinical waste. The area is then cleaned with a detergent solution, followed by a TGA-listed disinfectant applied at the recommended concentration and left for the full contact time. Everything used in the clean-up goes into clinical waste. Hands are washed immediately after removing gloves.
The wipe technique matters during routine cleaning as well. Wiping in a tight S-shaped pattern from top to bottom and from clean to dirty areas prevents contamination from being spread across a surface rather than removed from it. It sounds like a small detail. On a high-touch surface that has been wiped dozens of times incorrectly, it is not.
Discharge and Terminal Cleaning After a Patient Leaves
When a patient or client has used a treatment room, recovery bay, or consultation space, the cleaning requirements intensify. Terminal cleaning, meaning the thorough cleaning and disinfection of a space after it has been occupied, covers all surfaces that the patient came into contact with or that may have been contaminated during their care. This includes the treatment surface, any shared equipment, the chair or bed, surrounding furniture, and frequently touched surfaces in the room.
In a general practice setting, this is more straightforward than in an inpatient facility, but the principle is the same. Rooms that have been used by a patient with a known or suspected infection need additional attention: a higher disinfectant concentration may be required, shared items like blood pressure cuffs need to be cleaned before use on the next patient, and any disposable items should be discarded rather than retained.
What Good Cleaning Equipment Practice Looks Like
Cleaning equipment itself can become a source of cross-contamination if it is not managed properly. Mop heads and reusable cloths that are used across multiple areas without being changed transfer organisms from one surface to another. In a clinical environment, microfibre cloths should be used for a single area or purpose and then laundered, not rinsed out and reused. Disposable cloths are the cleaner option in high-risk rooms.
Spray bottles and dry brooms are not appropriate tools for clinical cleaning. Spray bottles generate aerosols that can disperse pathogens and irritant chemicals into the breathing zone; dry brooms disperse dust particles rather than capturing them. Damp mopping or microfibre flat mopping with a fresh head per area is the standard.
Mop buckets should be emptied, cleaned, and allowed to dry after each use. Do not refill and reuse them. Cleaning solutions should be prepared fresh as needed; solutions that have been sitting in a bucket for hours lose their efficacy and can become contaminated.
A Note on Waiting Room Hygiene That Often Gets Missed
Waiting rooms are the entry point to your facility, and they are used by people who are often already unwell, elderly, immunocompromised, or bringing children in for care. The infection control risk is real, but waiting rooms are routinely cleaned to an office standard rather than a clinical one.
The reception counter, the EFTPOS terminal, any shared pens, and all seating armrests are clinical contact surfaces for cleaning frequency. They should be included in your high-touch surface cleaning schedule, not left until the end-of-day clean. If your waiting room has magazines or shared items, remove them. They cannot be reliably cleaned, and they represent an unnecessary transmission risk.
Getting Your Cleaning Program Right for a Care Setting
Effective infection control cleaning in a care environment is not about cleaning everything as aggressively as possible. It is about understanding which surfaces carry the most risk, what frequency is appropriate for each, and making sure the right products are used in the right order. A well-designed healthcare cleaning program is built around these distinctions, documented in a schedule that reflects the actual activity in your facility, and reviewed when local conditions change.
If you are not confident that your current cleaning arrangements meet medical centre cleaning standards, the place to start is an honest audit of your high-touch surfaces, and whether they are being cleaned at the frequency the clinical environment actually requires.

Adam Thomas is the Founder and CEO of NTFG, one of Sydney’s leading commercial cleaning companies specialising in childcare, healthcare, and education facilities. With over a decade of hands-on experience in infection control and hygiene management, Adam has developed cleaning protocols for hundreds of early learning centres across Sydney. He regularly consults with childcare operators on compliance, staff training, and outbreak prevention strategies.






